Phacoemulsification is a procedure in which the lens and the front portion of the capsule are removed. The cataract is broken up, or emulsified, into small pieces using an ultrasound tip. Phacoemulsification has gained in popularity in recent years, and is now the preferred form of cataract removal. The procedure is very popular and has refined over the years and has high success rate and shorter recovery periods. The procedure has constantly refined over the years to make it even safer and more successful. Innovations in technology such as the foldable IOL also have helped improve outcomes by allowing surgeons to make smaller incisions.
Diagnosis
Cataracts are there normally for years before vision is impaired. Surgery is recommended as the lens grows cloudier and vision deteriorates.
The common symptoms noted are:
Onset of blurred vision
Poor central vision
Frequent changes in corrective lenses
Increased glare from lights
Improved near vision
Poor vision in sunlight
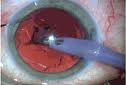
Cataracts grow faster in younger people or diabetics, so doctors will recommend surgery more quickly in those cases.
Surgery may also be recommended sooner if the patient suffers from other eye diseases such as agerelated macular degeneration and if the cataract interferes with complete eye examination.
When symptoms worsen to the point that everyday activities become problematic, surgery becomes necessary. A complete ocular exam will determine the severity of the cataract and what type of surgery the patient will receive. For some denser cataracts, the older method of extracapsular extraction is preferred.
The diagnostic exam should include measurement of visual acuity under both low and high illumination, microscopic examination of eye structures and pupil dilation, assessment of visual fields, and measurement of intraocular pressure (IOP). If cataracts are detected in both eyes, each must be treated separately.
Overall patient health must also be considered, and how it will affect the surgery's outcome. Surgeons may recommend a complete physical examination before surgery. Although preoperative instructions may vary, patients are usually required not to eat or drink anything after midnight the day of the surgery. Patients must disclose all medications to determine if they must be discontinued before surgery. Patients taking aspirin for blood thinning usually are asked to stop for two weeks before surgery. Blood-thinning medications may put patients at risk for intraocular bleeding or hemorrhage. People should consult with their eye doctor and internist to decide the best course of action.
An A-scan measurement is done to determine the length of the eyeball. This helps determine the refractive power of the IOL. Pre-surgical tests such as a chest x ray, blood tests or urine analysis may be needed if other medical problems are of concern.
An A-scan measurement is done to determine the length of the eyeball. This helps determine the refractive power of the IOL. Pre-surgical tests such as a chest x ray, blood tests or urine analysis may be needed if other medical problems are of concern.
Cataract surgery is done on an outpatient basis and patients are discharged the same day. Dilating eye drops, antibiotic drops and a corticosteriod or nonsteroidal anti-inflammatory drop may be used. Anesthetic eye drops will be given in both eyes to keep both eyes comfortable during surgery. A local anesthetic also will be administered. Patients are awake for the surgery, but are kept in a relaxed state.
The patient's eye is scrubbed prior to surgery and sterile drapes are placed over the shoulders and head. The patient is required to lie still and focus on the light of the operating microscope. A speculum is inserted to keep the eyelids open.
Procedure:
A local anesthesia is given by the surgeon through a long needle, usually inserted through the lower eyelid. This numbs the area behind the eyeball. A slight pressure will be given on the eyeball to help stop any bleeding caused by the anesthetic and decrease intraocular pressure, which lowers the chances of complications. An oxygen tube will help the patient breathe as the patient will be covered with drapes.
An operating microscope is used and the patient makes an incision os about 3 mm on the side of the anesthetized cornea. The site of incision varies depending on the size and extent of the cataract. A viscoelastic fluid is then injected to reduce shock to the intraocular tissues. The surgeon then makes a microscopic circular incision in the membrane that surrounds the cataract. A water stream then frees the cataract from the cortex. The surgeon inserts a small titanium needle, or phaco tip, into the cornea. The ultrasound waves from the phaco tip emulsify the cataract so that it can be removed by suction. The surgeon first focuses on the cataract's central nucleus, which is denser. In the first stages of a cataract, people may notice only a slight cloudiness as it affects only a small part of the lens, the part of the eye that focuses light on the retina.
During emulsification, the machine simultaneously aspirates the cataract through a small hole in the probe. The posterior capsule, which is used to support the intraocular lens will be left in place.
The folded IOL is inserted by an injector. After the IOL is inserted the viscoelastic fluid is removed. Sutures are usually not required and the patient would be adviced to wear an eye shield immediately after the surgery. The entire procedure takes about 20 to 30 minutes. Phacoemulsification allows cataract surgery to be performed through a very small incision in the cornea.
Aftercare:
The patient is advised to rest for at least 24 hours. Only light meals are recommended on the day of surgery. The patient may still feel drowsy and may experience some eye pain or discomfort. Usually, over-the-counter medications are advised for pain relief, but patients should check with their doctors to see what is recommended. Other side effects such as severe pain, nausea, or vomiting should be reported to the surgeon immediately.
There will be some changes in the eye during recovery. Patients may see dark spots, which should disappear a few weeks after surgery. There also might be some discharge and itching of the eye. Patients may use a warm, moist cloth for 15 minutes at a time for relief and to loosen the matter. All matter should be gently cleared away with a tissue, not a fingertip. Pain and sensitivity to light are also experienced after surgery. Some patients may also have slight drooping or bruising of the eye which will improve as the eye heals.
Patients have their first postoperative visit the day after surgery. The surgeon will remove the eye shield and prescribe eye drops to prevent infections and control intraocular pressure. These eye drops are used for about a month after surgery. Essentially all the advantages of phacoemulsification are because of small incision, which is self-sealing. phacoemulsification involves removing the eye's natural lens while leaving in place the back of the capsule, which holds the lens in place.
Patients are advised to wear an eye shield while sleeping, and refrain from rubbing the eye for at least two weeks. During that time, the doctor will give the patient special tinted SUNGLASSES or request that he or she wear current prescription eyeglasses to prevent possible eye trauma from accidental rubbing or bumping. Unlike other types of cataract extraction, patients can resume normal activity almost immediately after phaco.
About Eye
Eye Diseases
Vision problems
Find Cost
Surgeries & Treatments
Best Eye Hospitals
Testimonials
Get Free Quotes
Cataract Surgery
Intacs
Astigmatic Keratotomy(AK)
Canalicular Tear Repair
Chalazion Surgery
Conductive Keratoplasty(CK)
Corneal Transplantation
Lasik Surgery
Top Hospitals In India
Top Hospitals In Turkey
Top Hospitals In Mexico
Top Hospitals In Costa Rica
Top Hospitals In Singapore
Top Hospitals In UAE
Top Hospitals In Australia
Top Hospitals In Malaysia
Top Hospitals In Thailand
Top Hospitals In Phillipines